Covid Lockdowns - A Tale of Two Nations
What does the data tell us about the impact of the Autumn 2020 lockdowns in Wales and England
Summary.
This is the first of three posts that will look at the impact of the lockdown measures implemented in the UK during the period October 2020 to May 2021. A period when the UK home nations saw two separate period of lockdowns.
The aim of these posts is twofold. First does the data tell us anything about the impact these lockdowns had on deaths from Covid within and after the period they were implemented. And secondly, can we learn anything about the importance of the timing and duration of lockdowns.
This first post looks at the Autumn lockdowns implemented during October and November 2020 in Wales and England. It shows that we need to be careful drawing quick conclusions from simple analysis and finds that whilst these lockdowns stopped the rise in Covid deaths the effect was not sustained as mitigations relaxed and a new variant emerged.
Nobody wants lockdowns.
Governments do not take the decision to implement lockdown decisions lightly. The impact on society and the economy are huge and are best avoided through other measures. In the absence of a vaccine, effective contact tracing with isolation of infectious individuals, together with other measures like social distancing, offer a far better approach. Unfortunately, these measures are sometimes insufficient and lockdowns are implemented.
The perils of a simple analysis.
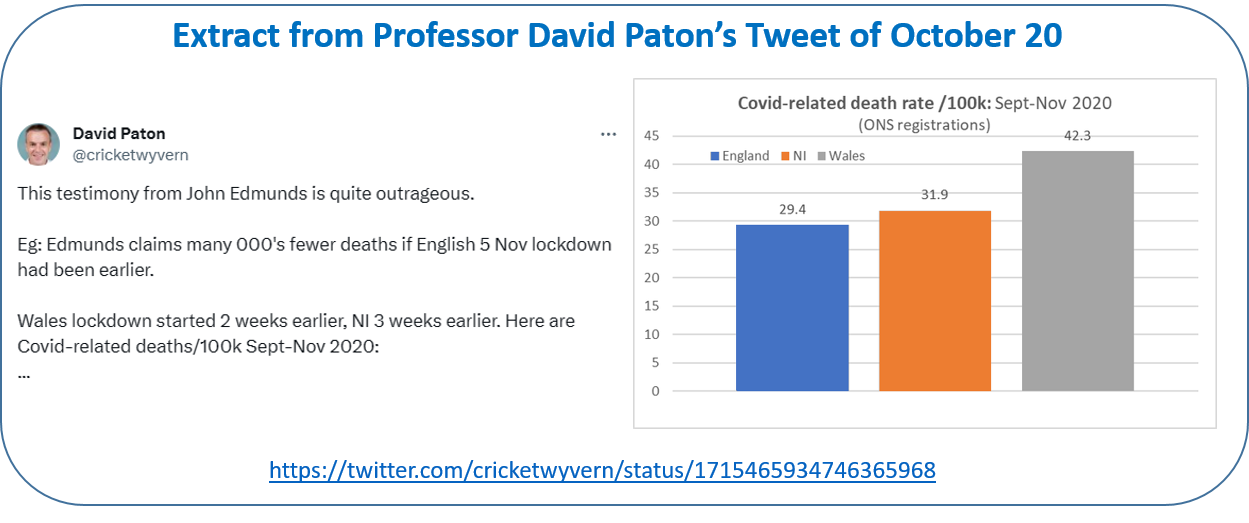
One of the motivations for this article was a tweet published by David Paton (Professor of Industrial Economics at Nottingham University). An extract from his tweet is shown below.
Professor Paton presents a graph comparing the Covid-related death rate/100k for England (blue), Northern Ireland (orange) and Wales (grey) for the period Sep–Nov 2020. He argues that as Wales entered lockdown 2 weeks earlier than England the significantly higher death rate in Wales confirms that locking down earlier in England would not have saved lives.
But is that the message that we can take from the graph? Well the short the answer is no and this is for two main reasons. First each of the home nation’s lockdowns was different – the situation ahead of the lockdown was different, the nature of their lockdowns was different, and the mitigations after the lockdown were different. Secondly, any analysis must account for the time lag between being infected and death.
Let’s start by looking at the impact of the time lag between getting infected for Covid and death. The time between getting infected and death typically ranges between 15 to 23 days (see Appendix 1 for a details). Consequently, as lockdowns aim to break the chain of infections the earliest we would expect to see any impact on deaths would be two to three weeks after the start of a lockdown. With Wales entering it’s ‘circuit breaker’ lockdown on October 23 the earliest any impact would be is after Nov 7. Consequently, Wales’s death rate for the period Sep to Nov 2020 tells us virtually nothing about the impact of the ‘circuit breaker’ as it could only have impacted 3 of the 13 weeks covered by this reporting period at most. Comparing it with the Sep-Nov 2020 death rates for England is not the compelling evidence that Professor Paton believes!
Is there a better way?
Although the analysis just discussed tells us little about the impact of lockdowns on deaths it is possible to learn something about their effectiveness from the data. But first we need to remind ourselves about the differences between the mitigations implemented by England and Wales during the second half of 2020. Fortunately, Oxford University documented the Home Nation’s responses to the pandemic and the following is an extract from a report they published in April 2021.
As you can see the two lockdowns were different. In summary, England entered it’s lockdown with stronger restrictions than Wales in some areas, had a longer lockdown, and came out of lockdown with slightly stronger restrictions.
With that context in mind let’s now look at the death rate for the two home nations. It’s important to remember that these charts only show deaths which are reported on death certificates as those due to Covid. Deaths where Covid was a possible contributing factor are not included.
The following chart shows the deaths per 100,000 by day of death for the period Sep 1 to Dec 31, 2020 for Wales. The two blue diamond markers indicated the number of days since the start of the ‘circuit breaker’ lockdown when we would start to see any impact on deaths. These are the estimated range of days between infection and death (Appendix 1 provides a detail description of the time from infection to death). Finally, the yellow shading indicates the timing and duration of the ‘circuit breaker’.
The chart shows that Wales entered their ‘circuit breaker’ on Oct 27 with a rapidly rising death rate from Covid which continued to increase throughout the 17 days when it was operational. After 15 days the death rate continued to rise but by day 23 the increase had stopped and plateaued before rising again in mid-December. Clearly the ‘circuit breaker’ halted the rise in the death rate when expected. However, it failed to reduce the death rate which remained at high levels.
I think that there are two main conclusions we can draw from this analysis. First, a 17 day ‘circuit breaker’ was effective at stopping the death rate rising but not sufficient to reduce it. A longer period of lockdown or stricter measures on lockdown exit was probably required. Whilst we can never be certain that this would have helped we will see later that there is evidence from England’s experience that supports this conclusion.
Secondly, the chart does not support the argument made by those opposing lockdowns that people will take actions to mitigate the spread of Covid before government implement lockdowns. If this was the case then death rates should have stopped rising much earlier. Indeed other data shows that Covid cases in Wales continued rising at the same rate until peaking on Oct 30 some 7 days after the start of lockdown and two weeks before the death rate stopped increasing.
Let’s now look at England’s data to see what we can learn.
The following chart shows the deaths per 100,000 by day of death for the period Sep 1 to Dec 31, 2020 for England. Again the two blue diamond markers indicated the number of days since the start of the lockdown which is when we would expect to see any impact. The grey shading represents the timing and duration of the lockdown.
Interestingly, England entered its lockdown with almost exactly the same death rate as Wales had when it implemented their ‘circuit breaker’. This is important because it shows that comparing calendar dates for the two lockdowns is not meaningful. In terms of the ‘Covid calendar’ England and Wales entered their lockdowns on the same ‘Covid day’ with death rates of 0.55 deaths per 100,000.
The overall impact of England’s lockdown follows a very similar pattern to Wales. The death rate peaks when expected on Nov 22 some 17 days from the start of lockdown, has a short plateau before starting to increase from mid-December.
However, there is one significant difference as England comes out of lockdown with a much lower death rate than Wales despite both entering there lockdowns at the same level. This is probably because England had a longer lockdown and higher levels of mitigations than Wales after lockdown. However, Wales had a much faster growth rate (8 day doubling) than England (18 day doubling) immediately before they entered their respective lockdowns which may also explain the difference.
To understand more we need to look at what happened at a regional level in England. In my next article I will be taking a deep dive in to what happened during the Autumn lockdown in the different English regions. It makes for an interesting story and shows that a new variant was starting to show its’ presence in the Autumn Lockdowns.
To summarise …..
I hope that in this short article I have shown some of the challenges in comparing different countries experiences especially when drawing conclusions about the impact of lockdowns. It’s easy to get misled without an understanding of the context around each lockdown and the time lag between infection and death.
Finally, whilst both lockdowns slowed the rate of death for a while and undoubtable saved lives they only succeeded in stabilising the death rate for a relatively short time before continuing to increase.
On this latter measure the lockdowns were not as successful as the policy-makers would have anticipated. However, we will see in the next article that a new variant, unknown at the time, was already starting to change the situation for the worse.
Appendix 1. Estimating the time between Covid infection and death
The duration between a COVID infection and death can vary depending on several factors such as the severity of the infection, age, and underlying health conditions of the infected person. Most studies report the time between symptom onset and death so it is necessary add the time between infection and symptom onset which on average is 5 days.
A review from the Office for National Statistics, based on early studies using data from China, reported that median times between symptom onset and death were between 16 to 19 days. However, a later study by CO-CIN found that the time from symptom onset until death in UK hospitalised patients was between 7 to 13 days.
These studies show a quite large range so I have taken the average of the two median times of symptom onset to death from each study to calculate a lower (10 days) and upper (18 days) value. Adding the average 5 days from infection to symptom onset gives an estimated range of 15 days to 23 days for the time between Covid infection and death. It is these values that are used in the analysis.
Finally, Adam Kucharski, from the London School of Hygiene and Tropical Medicine, highlights a subtle but very important point that needs careful consideration when ‘interpreting timing of changes in infection (and transmission) from subsequent clinical outcomes.’ In a Sep 2022 tweet, he gives a worked example showing that a sharp fall in infections shortened the observed time between the peak of infections and the peak of reported outcomes (e.g. deaths) below what would be expected.
This rather counter-intuitive finding is illustrated in the two graphs shown below. The left hand graph gives the distribution of the time between infection to outcome with an average of 25 days. Intuitively, we would expect to see a 25 day lag between a change in infections and a change in outcome, and this is what we normally see. However, a sharp abrupt reduction in infections, as we would expect when implementing a lockdown, changes this normal behaviour and reduces the time lag between the peak of infections and the peak of outcomes. This is shown in the right hand graph where a sharp decline in infections (black line) results in a decline in the reported outcome (red line) some days later. In this modelled example it is 17 days between the two peaks not the expected 25 days.
This is because infections drop off sharply in this scenario, the timing of the peak in clinical outcomes will be influenced by the cumulative shapes of all the delayed outcomes of the infections, the bulk of which occurred before the fall in infections.
In the worked example we see a change in reported outcomes 8 days earlier than the average number of days between infection and outcome. This is quite a significant ‘pull-ahead’ but it’s important to note that the result is determined by the spread of the delay from infection to outcome (the wider the spread the longer the ‘pull-ahead’) and how quickly the infections fall. Separately, I have modelled the ‘pull-ahead’ for a delay from infection to death of 25 days using a normal distribution with a standard deviation of 5 days and a less abrupt declines in infection. These showed a ‘pull-ahead’ of 2 to 3 days which is within the ranges used in my analysis.